Bladder Prolapse
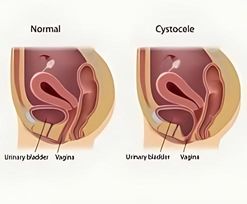
Bladder Prolapse
Bladder prolapse, also known as cystocele, occurs when the bladder drops from its normal position and bulges into the vaginal wall. This happens due to weakening of the pelvic floor muscles and supportive tissues, often as a result of childbirth, aging, menopause, chronic straining, or prior pelvic surgeries.
While bladder prolapse is not life-threatening, it can cause significant discomfort, urinary problems, and impact a woman’s quality of life. The condition varies in severity, from mild cases with minimal symptoms to advanced prolapse requiring medical or surgical intervention.
Signs & Symptoms
- A bulge or pressure sensation in the vaginal area
- Frequent urinary tract infections (UTIs)
- Difficulty emptying the bladder completely
- Urinary leakage (incontinence) during coughing, sneezing, or physical activity
- Increased urinary frequency or urgency
- Pain or discomfort during intercourse
- Lower back or pelvic pain
- Feeling of heaviness or pulling in the pelvis
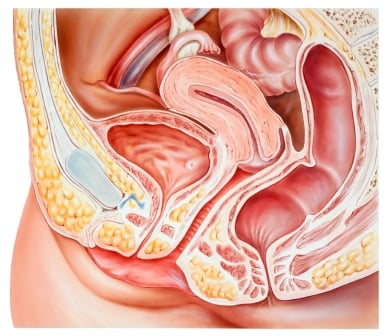
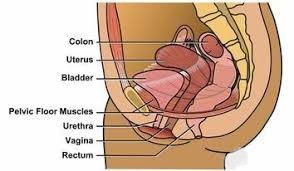
Diagnostic Procedures
- Medical History & Physical Examination: To assess pelvic support and severity of prolapse.
- Pelvic Examination: Done with the patient standing or straining to visualize the prolapse.
- Urine Flow & Residual Tests: To check bladder emptying efficiency.
- Ultrasound / MRI (if needed): For detailed imaging of pelvic structures.
- Cystoscopy (in select cases): To examine the bladder lining and rule out associated issues.
Why Choose UROSQUARE MEDICAL SERVICES LLP. for Bladder Prolapse Care?
- Specialized Urology & Women’s Health Center – Dedicated expertise in managing pelvic organ prolapse with the latest medical and surgical approaches.
- Comprehensive Female Urology Services – Focus on conditions unique to women, with a patient-friendly and confidential environment.
- Advanced Diagnostic Tools – Use of cutting-edge imaging and endoscopic technology for precise evaluation.
- Personalized Treatment Options – From pelvic floor physiotherapy and pessary fittings to minimally invasive reconstructive surgeries.
- Multidisciplinary Care – Collaboration between urologists, gynecologists, physiotherapists, and pelvic health specialists for holistic management.
- Patient-Centric Approach – Compassionate counselling, clear communication, and long-term follow-up to ensure sustained well-being.

